While previous systematic reviews have found eating red and processed meat is associated with overall or cardiovascular mortality (1), these analyses have suffered from methodological limitations. Often, such reviews have failed to consider the quality of the reviewed evidence or the magnitude of the observed relationship. This paper — one of five published by this research team (2) — provides an updated review of these associations.
The researchers collected data from large cohort studies (of at least 1,000 adults) assessing the relationship between red and/or processed meat intake and cardiovascular or all-cause mortality. Sixty-one studies covering over four million subjects met these criteria.
The GRADE methodology was used to assess the certainty and strength of any observed associations. In brief, GRADE uses the following factors to evaluate the certainty of an evidence-based judgment:
- Study design (e.g., observational, randomized controlled trial)
- Consistency and magnitude of effect (including the existence, or lack thereof, of a dose-response relationship)
- Precision of measurement of both inputs (e.g., dietary consumption patterns) and outputs (e.g., heart disease and mortality outcomes)
- Risk of bias in the surveyed trials
The associations between reducing red and/or processed meat intake (i.e., consuming three fewer servings per week) and mortality and/or cardiovascular outcomes are shown in the tables below.
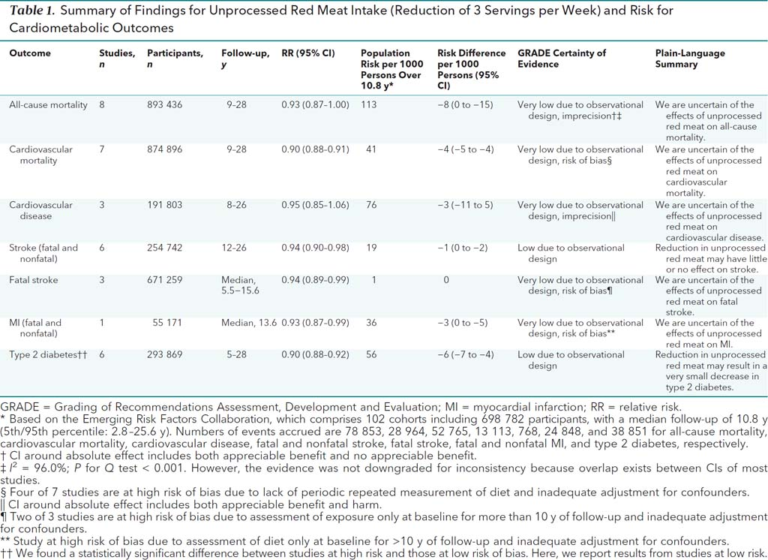
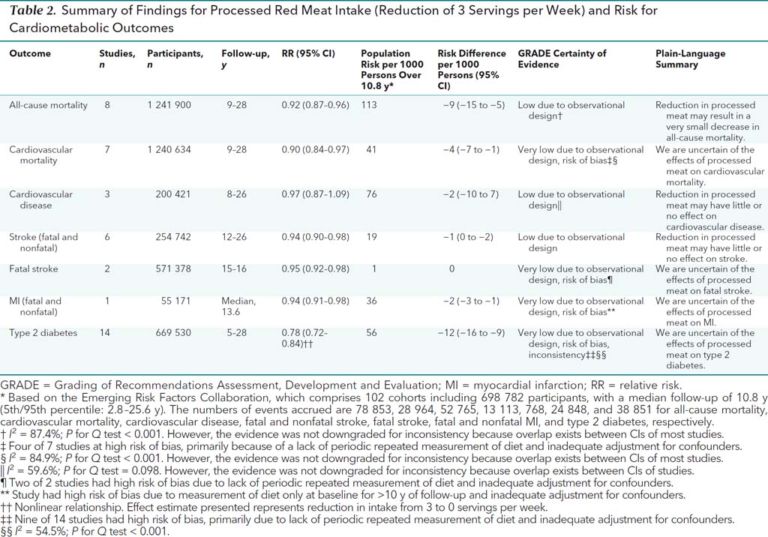
In sum:
- There was no significant association between a reduction in red meat consumption and overall mortality.
- There was a statistically significant association between a reduction in red meat intake and cardiovascular mortality and cardiovascular disease. The magnitude of these outcomes, however, was very small — a reduction in red meat intake was associated with four fewer cardiovascular deaths per 10,800 person-years.
- As assessed by GRADE, the certainty of these associations was low or very low. Many trials failed to accurately assess meat intake over time (often assuming a single point estimate of meat intake reflected eating patterns over months or years) and/or failed to adjust for potential confounders.
- Similar results were seen for processed meat consumption, with statistically significant but low-magnitude and low-certainty associations between a reduction in intake and improvements in cardiovascular or mortality outcomes.
A separate review by these same authors found dietary patterns containing red and/or processed meat showed similar associations with cardiovascular and/or mortality outcomes (3). The authors interpret this as suggesting red meat may not be directly driving increased risk and instead may be a marker for unhealthy eating patterns.
Overall, the researchers found the evidence supporting any association between red and/or processed meat and cardiovascular or mortality outcomes to be of a consistently low quality. If reducing red and/or processed meat has any impact on mortality, the impact is very small.
Notes
- E.g., “Food groups and risk of all-cause mortality: a systematic review and meta-analysis of prospective studies”; “Association between total, processed, red and white meat consumption and all-cause, CVD and IHD mortality: a meta-analysis of cohort studies”; and “Red and processed meat consumption and mortality: dose-response meta-analysis of prospective cohort studies.”
- See “Effect of lower versus higher red meat intake on cardiometabolic and cancer outcomes. A systematic review of randomized trials”; “Reduction of red and processed meat intake and cancer mortality and incidence. A systematic review and meta-analysis of cohort studies”; “Patterns of red and processed meat consumption and risk for cardiometabolic and cancer outcomes. A systematic review and meta-analysis of cohort studies”; and “Health-related values and preferences regarding meat consumption. A mixed-methods systematic review.”
- See “Dairy intake revisited—associations between dairy intake and lifestyle related cardio-metabolic risk factors in a high milk consuming population,” and “Patterns of red and processed meat consumption and risk for cardiometabolic and cancer outcomes. A systematic review and meta-analysis of cohort studies.”